Relationships and sexual satisfaction are important to quality of life. This is especially true for people coping with chronic illness.
Courtesy of the Amyotrophic Lateral Sclerosis Society of Canada
Sex is an act that can bring satisfaction and release. Even though ALS does not directly affect sexual function, for a person with ALS, sex may also bring pain, frustration and embarrassment. There are methods and techniques available to help people with ALS and their partners cope with their changing sex life and maintain intimacy. “Sexual health is the integration of the somatic, emotional, intellectual, and social aspects of sexual being, in ways that are positively enriching and that enhance personality, communication and love.”
World Health Organization, Report Series 572; Geneva, 1975
Benefits of sex
Chronic illness can restrict the activities of daily living. Maintaining a sexual relationship can be a source of comfort, pleasure and intimacy and an affirmation of one’s true self when other roles have been stripped away. A satisfying sex life, for the person with ALS and their partner, is one way to feel “normal” when so many other areas in their lives have changed. Documented benefits of sex include:
• Orgasm frequency is inversely related to risk of death
• Reduction of stress
• Improved sleep post-orgasm
• Increased relationship satisfaction and stability
Sexual response cycle and chronic illness
Understanding the sexual response cycle is important to understanding the impact that chronic illness can have on sexual functioning. Sexual function, or dysfunction, is a combination of physical (due to disease-specific changes or medication, or both) and psychosocial factors. Any illness or treatment that affects these factors can have a negative impact on a person’s ability or desire to engage in sexual activity.
Effects of ALS on sexuality
Chronic illness can affect sexual satisfaction and the sexual relationship for both partners. ALS does not impair sexual function but medications, immobility, respiratory problems, fatigue, and body image factors may negatively affect sexuality.
Biological effects
• The effects and side effects of some medications can reduce sexual desire and/or the ability to have intercourse or orgasm.
• Reduced cardiovascular and pulmonary function, fatigue or pain can limit sexual activity.
• Medical treatments may alter the person’s appearance and bodily function. Psychological distress caused by these changes can limit sexual satisfaction. For instance, people with ALS may feel less desirable if they are using a ventilator or have a feeding tube.
 Psychosocial effects
Psychosocial effects
• Anxiety, loss of self-esteem, grief and depression associated with chronic illness may impair sexual fulfillment.
• Chronic illness alters relationship dynamics. Partners become caregivers as well as lovers. Role changes may cause sexual activity to decrease.
Social effects
• Society is uncomfortable with the idea of ill people wanting to have or having sex.
• Although sexual activity may be placed on hold intermittently during the illness, sex remains a vital part of day-to-day living for some people with chronic illness.
How can you keep your sex life healthy? Read about your illness. Be informed. Know your body and what feels right in your current state.
Suggestions to help you prepare for sexual activity
• Plan sexual activity for the time of day when you have the most energy and your health problems are least intrusive.
• Be sure you are rested and relaxed.
• Wait at least two hours after eating to have sex.
• Take any required pain medication 30 minutes before sex.
• Alcohol and tobacco can affect sexual function.
• Reduce or stop taking medications that have a negative impact on sexual functions before sexual activity (on the advice of a physician). “Sex is more than an act of pleasure, sex is the ability to be able to feel so close to a person, so connected, so comfortable that it’s almost breathtaking to the point you feel you can’t take it. And at this moment you’re a part of them.”
– Sophia Loren
Suggestions to help you maintain a healthy sex life
• Try alternative ways to experience sex and sensuality. Hold hands, hug, touch your partner and initiate physical contact, even when you do not plan to have sex. ALS does not affect your sensory nerves.
• Use your senses to make sexual activity more enjoyable.
• Communicate with your partner. Be honest and open. Tell your partner what you like and do not like.
• Try different sexual positions to accommodate your body’s changing abilities. Experiment with positions that minimize weight bearing or tiring movements.
• If you are in a wheelchair, consider a model with removable arms.
• Use a waterbed to relieve pressure on joints and to minimize weightbearing positions.
• Try personal lubricants to reduce discomfort during intercourse.
• Book appointments for sex with your partner. Conserve your energy and save it for some intimate time with your partner.
• Consider either self-stimulation or mutual stimulation. Although not acceptable to all people, this provides another method for you and your partner to pleasure one another.
Orgasm produces a natural high. It helps with pain control and stimulates pleasure producing chemicals in the brain.
“The intimacy in sex is never only physical. In a sexual relationship we may discover who we are in ways otherwise unavailable to us, and at the same time we allow our partner to see and know that individual. As we unveil our bodies, we also disclose our persons.” Dr. Thomas Moore, “Soul Mates,” Psychology Today, (Mar/Apr 1994), pp. 28, 29.
Therapies and suggestions to help the person with ALS during sexual intimacy
• Trapped in a body that ceases to respond, too much time to think, sex can be very enjoyable, as everything works fine. If desires are left unsatisfied, sex can become one more adverse and painful agony to deal with. It shouldn’t be that way.”
– person living with ALS
People with ALS may feel depressed or tired a lot of the time. They may experience pain, weakness, difficulty breathing, problems with co-ordination and trouble sleeping. However, there are ways to combat these issues so that both the person with ALS and their partner can engage in sexual activity.
Spasticity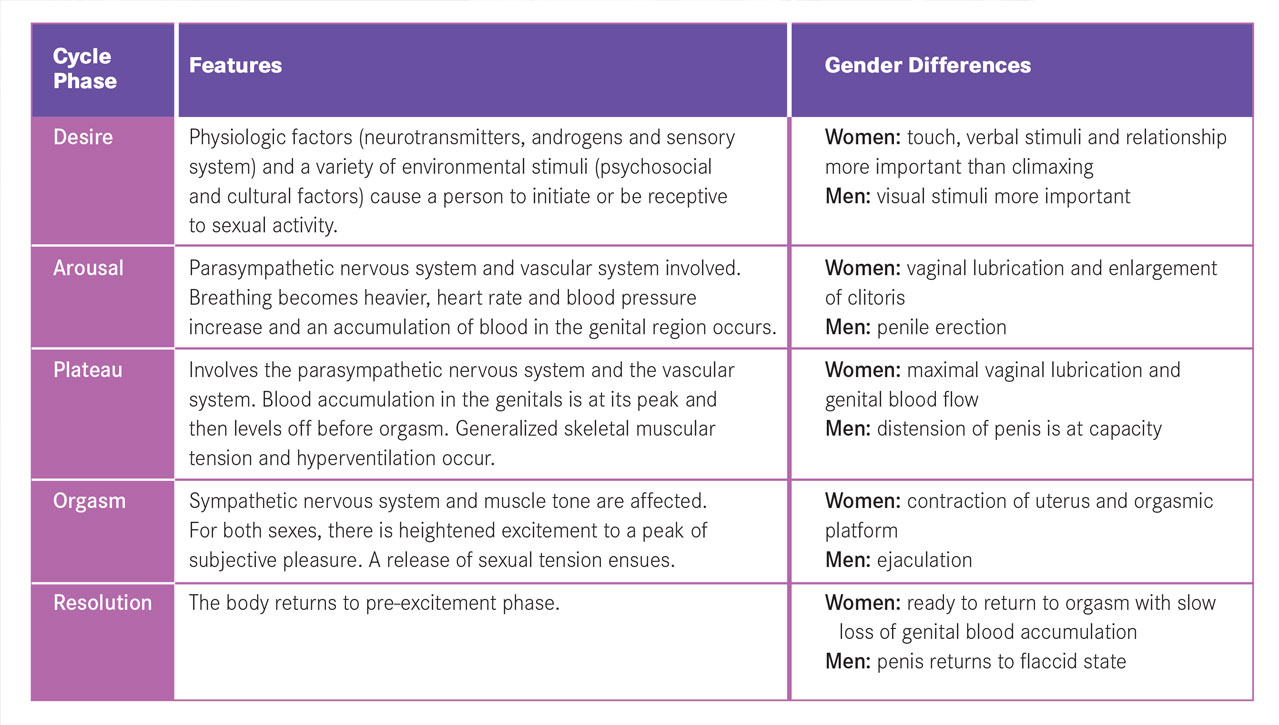
(a disorder in which certain muscles are continuously contracted)
• Experiment with sexual positioning
• Take a warm bath prior to having sex
• Consistently ice sore areas
• Use antispasticity medicines (talk to a doctor about this)
• Massage/stretching and support of joints
Spasticity during sex can be embarrassing, frustrating and challenging, especially since sexual arousal itself may cause spasms. Bathing in warm water prior to sexual activity may reduce spasticity and relax muscles and joints. The relaxing effects of sex play can help to reduce spasticity and allow for penetration, if desired, once joints and muscles are calmed.
Positioning for the individual with spasms
• For men who are unable to straighten their legs, an effective position is with the man on his back, partner on top. The partner can lean back against his bent legs.
• The individual can lay on their side with a pillow or towel between the legs. This position is especially useful when there are knee or hip contractures. Spoon entry from behind works well with this arrangement.
Mobility
• Use adapted orthoses, lifts and positioning devices
• Employ sexual aids and toys; vibrators with hand straps
• A third party intervention can help position both partners
The individual with ALS often experiences compromised mobility. Adaptations to sexual positions and techniques may be required. Yet, sexual activity can continue to occur and to be satisfying. Sex does not need to involve penis-in-vagina penetration. Penetration does not have to involve the penis. Individuals who are unable to penetrate their partners can employ fingers, hands and sex toys instead. The intimacy and body-to-body contact that comes with penetration can still be reached through other methods:
• Fingering (using the fingers to penetrate your partner)
• Vaginal fisting (insertion of the entire hand into your partner’s vagina)
• Harnesses and dildos can be used to explore vaginal penetration. Men can choose from two kinds of strap-on toys. The first fits over your penis and straps around your waist. The second is a harness that leaves the penis exposed and places the dildo above your penis.
To counteract motor and sensory deficits
• Increase mental arousal (play music, meditate, practise visualization before sex)
• Increase genital stimulation (practise on self and then transfer to a partner situation)
• Use a personal lubricant
• Practise positioning prior to sexual activity
• Explore new ways to pleasure one another without being orgasm-oriented
• Use sight, sounds and smells. Expand your sexual repertoire to include oral/genital sex, fantasy and sensory experience.
Communication
• Develop a system for signaling desire and feedback during activity and direction
• Prepare advance voice recordings for communication aids
• Teach your partner how to use these aids during sexual activity
Bladder and bowel issues
• Maintain good hygiene
• Empty the bladder before sex
• Employ sexual positions that remove bladder pressure
• Decrease fluid intake two to three hours before sex
• Reposition the catheter to ensure proper function
• Use bladder medication 30 minutes prior to sexual intercourse
Positioning for the individual with ALS and partner
One partner on top
One partner lays on their back with pillows under the knees to keep the legs slightly bent. A rolled-up towel under the back will also work. This position works for almost all sexual activity.
Another position is for one person to lay on their front with a pillow under the hips or belly.
The partner who has more strength and control may take the position on top with their partner on their back or side.
Accommodations for a wheelchair/commode chair
A wheelchair with removable armrests offers numerous possibilities:
• Partner on lap facing you with their legs on either side
• For penetration, the partner can sit on the lap of the person in the wheelchair, facing away for a rear-entry position. They can use their arms to support themselves, leaning on your knees.
Wheelchairs without removable arms require different positioning for the partner:
• Partner sits on your lap facing away from you. The armrests can be used for support.
One partner lying on their side
Lying side-to-side is especially effective for an individual wearing a catheter. Both partners can move around without feeling encumbered.
Side positions can be used with partners facing one another. This allows both partners to engage in the thrusting movement.
When leg or hip tendons or muscles are tight, one partner lies on their side. The other lies perpendicular to their partner with their knees bent over their partner’s waist. This is a comfortable position that allows for long and slow penetration sessions.
The mind is the biggest sexual organ. Attitude is everything when dealing with chronic illness and sexuality. Yet, it must be nurtured so that a sexual relationship may occur. The following three sexual rehabilitation principles may help maintain a sexual and intimate relationship:
• Maximize the physiology (i.e., reduce fatigue, pain) to achieve optimal sexual benefits
• Adapt to limitations and make adjustments where necessary
• Stay positive and open to experiences.
Source: Amyotrophic Lateral Sclerosis Society of Canada.
References available upon request.














