How your assessment guides equipment choice
By Andree Gauthier, OT Reg (Ont)
The first Invacare Seating Rounds of 2013 was held this past February with approximately 60 therapists in attendance. Attendees had the opportunity to break out into smaller sessions where facilitators from three different areas of practice shared their own process of assessment.
Small sessions were run by:
Brenlee Mogul-Rotman, OT Reg (Ont), working in private practice; and Zach Bennett, HBSc, a rehab sales specialist at Motion Specialties Ltd.; who focused their session on seating and mobility assessments within the community setting.
Marlene Holder, PT, of Holland Bloorview Kids Rehabilitation Hospital; and Christel Meisinger, BKin, rehab mobility consultant from Motion Specialties Ltd.; who facilitated the session on assessment considerations for the paediatric client.
Andree Gauthier, OT Reg (Ont), of Toronto Rehab Institute’s Lyndhurst Centre; and Jeremy Dignard from Hunts Healthcare; who led the session on assessing clients within a seating clinic setting.
Assessment is “the process of gathering sufficient information about individuals and their environment in order to make informed decisions about intervention.”1 Any therapist involved with prescribing mobility and positioning devices must complete a comprehensive assessment. This assessment should move through predictable stages, should involve the consideration of many client factors, and should be accurate enough to lead to clear goals and successful interventions. In simple terms, “Assess and don’t guess.” The client, vendor, therapist and funding source all put in a large amount of resources (time, money) to obtain the equipment that best matches the client’s needs. That effort should not be wasted: the chosen mobility device should instill confidence, independence and safety, and not cause frustration, dependence and/or fear.
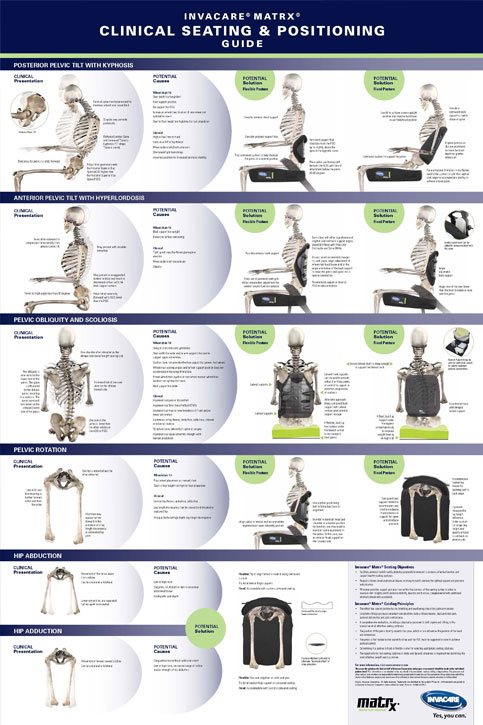 Seating and mobility in the community setting
Seating and mobility in the community setting
The community setting poses many challenges when completing a seating assessment. Some home environments are not set up for conducting a physical mat evaluation. There could be safety risks for the therapist such as a cluttered or infested apartment, unknown people within the apartment, or location in an unsafe neighborhood. Regardless of the challenges imposed, a full assessment is required and needs to be completed.
That being said, the in-home assessment should not proceed if either the therapist or the vendor feels they are in danger. It is important to review the risks involved with the vendor; consideration should be given to how and where the client can best be assessed. One recommendation is to arrange for both vendor and therapist to go together to the client’s home.
Another suggestion is to arrange for the client to meet at the vendor’s facility. Many vendors have their own assessment rooms, with proper mats, ceiling lifts and showrooms full of equipment, allowing for the assessment and mat evaluation to be conducted in a more supportive and safe environment. Also, discussion about equipment options and features may be easier since some products may be readily available to show the client.
It should be noted, however, that there are also advantages to visiting someone’s home. Such visits provide the therapist with the opportunity to observe environmental access in all areas of the home, and ascertain the client’s intended use of the equipment. The therapist will have the opportunity to observe first-hand the client’s functional level as they use a wheelchair in activities of daily living such as transfers on and off various surfaces, reaching for items and opening doors. So much information is required and can be gathered only by following a process. Accurate, robust information from the start reduces wasted time and usually rules out many equipment options right off the bat.
The seating and mobility assessment for children
With the paediatric population, it is very important to obtain clarity around the referral. Who referred the child and for what purpose? It is also important for therapists to remember that when working with a child, they have multiple clients: the parents, school and caregivers all have input into the child’s mobility needs. Even the child’s medication list will give clues to medical history that may not have been conveyed (e.g., spasticity, seizures). Information on past and upcoming surgeries needs to be determined. Children also present with various levels of vision and visual fields. What good is a headrest if the child has to twist around it in order to see? Pulmonary function may require extra machines to be carried on the chair, or specific positioning. The therapist has to determine how and where the mobility device will be used. How will the device and child be transported in the various vehicles used (such as the school bus, family car, grandparents’ car)? So much information is gathered even before the therapist moves onto a mat evaluation. However, equipment parameters and options will start to fall into place as more information is gathered.
The seating clinic setting for adults
These seating clinics usually follow clients with complex seating and mobility needs that cannot be met within the community. The client may require custom seating or specialized drive controls, or have chronic postural or skin issues where past interventions have been unsuccessful. Therapists working in a clinic setting usually have years of experience, and specialize in seating and mobility issues. The environment is usually supportive with equipment resources, access to other health care professionals for consults, and easy access to other seating and equipment specialists. Because most clinics are in a hospital setting, a doctor’s referral is required. Attending a seating clinic will require the client to travel and attend multiple appointments. This can be a challenge for some people.
Common to every setting
Many therapists may not have seating experience or consistent opportunity to gain experience in seating. They become unsure and lose confidence. It is recommended that they call on peers, vendors and manufacturers to assist in both learning and completing the assessment process.
• It is very important for therapists to communicate and ask questions.
• Therapists (and vendors) are obligated to find information, attend courses and educate themselves.
• Therapists have to complete their own funding forms and cannot hand them to the vendor to complete.
• Therapists should never sign their name to anything unless they agree with and understand it, and have completed it themselves.
A full comprehensive assessment will narrow down equipment choices and highlight required equipment parameters. It is not realistic for the client to try every backrest, cushion or wheelchair. Clinical findings help eliminate many options and narrow down choices. Taking accurate measurements, with vendor and therapist measuring the client together, will eliminate any discrepancies. It is crucial to communicate with the client/family about funding procedures and the payment process prior to receiving equipment. A clear discussion of delivery times, trial periods and rental options will avoid any disappointment.
An organized process
It is so important to find and follow an assessment form. This helps the therapist gather relevant information in all areas of a client’s life when living from a wheelchair. It helps keep the process organized, thorough and complete when there are distractions or discussions that pull the assessor’s attention in another direction. Even if a client is requesting replacement of old equipment with a similar, newer model, the full assessment should be completed. This is key in determining whether that same piece of equipment is meeting or still meets the client’s postural, mobility or skin needs. It may even pick up early signs of new issues that may require intervention. This same assessment should be completed even for equipment that may be considered “simple” to prescribe. For instance, if a client is requesting a scooter, the assessment will determine if the person has enough sitting balance for a basic seat and if specialized seating is required. It also helps to organize and collect relevant information for justification to funding agencies.
During the mat evaluation, assess a client’s range of motion, but also note the quality of their movement. When assessing hip range, the tendency to externally or internally rotate can give clues on what medial and lateral thigh contouring is required in a cushion. Assessing for ankle range will determine whether standard composite footplates are enough or whether angle adjustable plates will be required. A client with good sitting balance may require nothing more than a low back with minimal lateral support. While the client is out of the chair, the therapist will be able to take measurements and simulate where the support is required, and come out with the parameters for a potential backrest. Use hand simulation to determine what and where forces from the supports are required and in what direction. Will the client require custom seating? What about growth?
Issues such as sliding in a chair cannot be solved until the therapist discovers the cause. This can be determined only during a full assessment of the client. They will slide if they do not have the hip range, or if they have a kyphosis and the shape of their back does not match that of the backrest. If they have limited range in their neck due to kyphosis and their gaze is downward, they will have to extend at the hip to see who is talking to them, and then they will slide. The list of reasons can go on. See “Examine current equipment use” sidebar for more pointers on conducting an assessment.
Take-home message
A seating and mobility assessment must be completed in every setting; it is best practice, client centred and evidenced based. It helps formulate hypotheses on the source of any seating or mobility issues. It allows for equipment parameters to be effectively described and justified because it takes the guesswork out of the selection process. So please assess and don’t guess!
Andree Gauthier, OT Reg (Ont), has more than 20 years of experience in various settings and has spent the past eight years with the Toronto Rehabilitation Institute (TRI), Lyndhurst Centre in their outpatient seating clinic.
Photos: Invacare Canada














