What successful COVID-19 immunization efforts taught us about improving vaccine coverage among older Canadians for other vaccine-preventable diseases.
1) Vaccine hesitancy is low among older Canadians
Prior to the COVID-19 pandemic, it was believed that around 19% of Canadians considered themselves to be vaccine hesitant. Vaccine hesitancy is the ‘delay in acceptance or refusal of vaccines despite availability of vaccination services.’ Vaccine hesitancy exists on a continuum between those who accept all vaccines with no doubts and those who outright refuse all vaccinations with no doubts. Vaccine hesitant individuals fall into heterogeneous groups between these two ends of the continuum and can be broadly categorized into three groups: those who accept all vaccines but are unsure of or not fully confident about the decision, those who accept some vaccines while refusing others or delay vaccination, and those who refuse all vaccines but may have some doubts about this decision.
The reasons for vaccine hesitancy and vaccine uptake are complex and research shows that a range of characteristics are involved in older adults’ vaccine behaviours. The drivers of vaccine hesitancy or acceptance include psychosocial, socio-demographic, contextual, and physical factors. In addition, the kinds of factors that prevent or promote vaccine uptake can vary in type and significance depending on the particular disease and/or vaccine. The vaccine hesitancy continuum reflects the fact that there are multiple forms of vaccine hesitancy and that where individuals fall on the continuum can change over time as their knowledge, attitudes and behaviours in the context of vaccines evolve.
Canadians have shown a strong willingness to get COVID-19 vaccines. As of November 6, 2021, 89% of the eligible population has received one dose of a COVID-19 vaccine and 85% are fully vaccinated. As of November 6, 2021, 93% of Canadians aged 60 years and older have received at least one dose of a COVID-19 vaccine and 91% have been fully vaccinated with both doses.
The opportunity: This finding has implications for vaccine-preventable diseases such: as influenza, pneumonia, and shingles. As illustrated, these diseases have a significant impact on older adults, resulting in a substantial number of preventable hospitalizations and deaths annually. The best practices and actions from our COVID-19 vaccine rollout should immediately be applied to other immunization campaigns to better protect older adults.
2) Providing ample education about the risks of COVID-19 to older Canadians was key to increasing awareness about the importance of vaccination
During the COVID-19 pandemic, the risk of contracting COVID-19 and the severe health consequences for older adults living in both long-term care settings and in the community became well-known to the public. Canada’s long-term care crisis highlighted that older adults in congregate settings are especially vulnerable to contracting the disease. Long- term care and retirement homes were the epicenter of the COVID-19 pandemic in Canada, accounting for nearly 70% of the country’s deaths between March 1, 2020, and February 15, 2021.
Older adults are at higher risk of severe illness, complications, and death from COVID-19 due to both the physiological changes associated with ageing (such as a weakened immune system) and the propensity to have multiple pre-existing health conditions.
As such, older Canadians were disproportionately impacted by the COVID-19 pandemic and to this day still account for about 62% of hospitalizations and 93% of deaths in the country.
The heightened visibility of the COVID-19 pandemic instilled among older Canadians an awareness about the consequences of the disease which, in turn, likely led to an increased understanding about the importance of vaccination. Support for this comes from the fact that most older Canadians were willing to get vaccinated against COVID-19 long before vaccines were available = 86% of Canadians aged 65 and older reported that they would likely get a COVID-19 vaccine once one became available and more likely to follow other safety precautions like masking, distancing and testing. They were also more willing than younger folks to get a vaccine once Canada’s rollout began. The same trend was true internationally, with data from 19 countries with perceived susceptibility, perceived disease severity, and disease-related worry among the key predictors vaccine intentions. No surprisingly once vaccines became available, over 90% of older Canadians chose to get vaccinated within the first seven months of the rollout, achieving the highest coverage of any age group.
The opportunity: If public awareness about the disproportionate impacts of influenza, pneumonia, and shingles on older adults were comparable to the public understanding of COVID-19, vaccination rates against all three of these diseases may increase significantly.
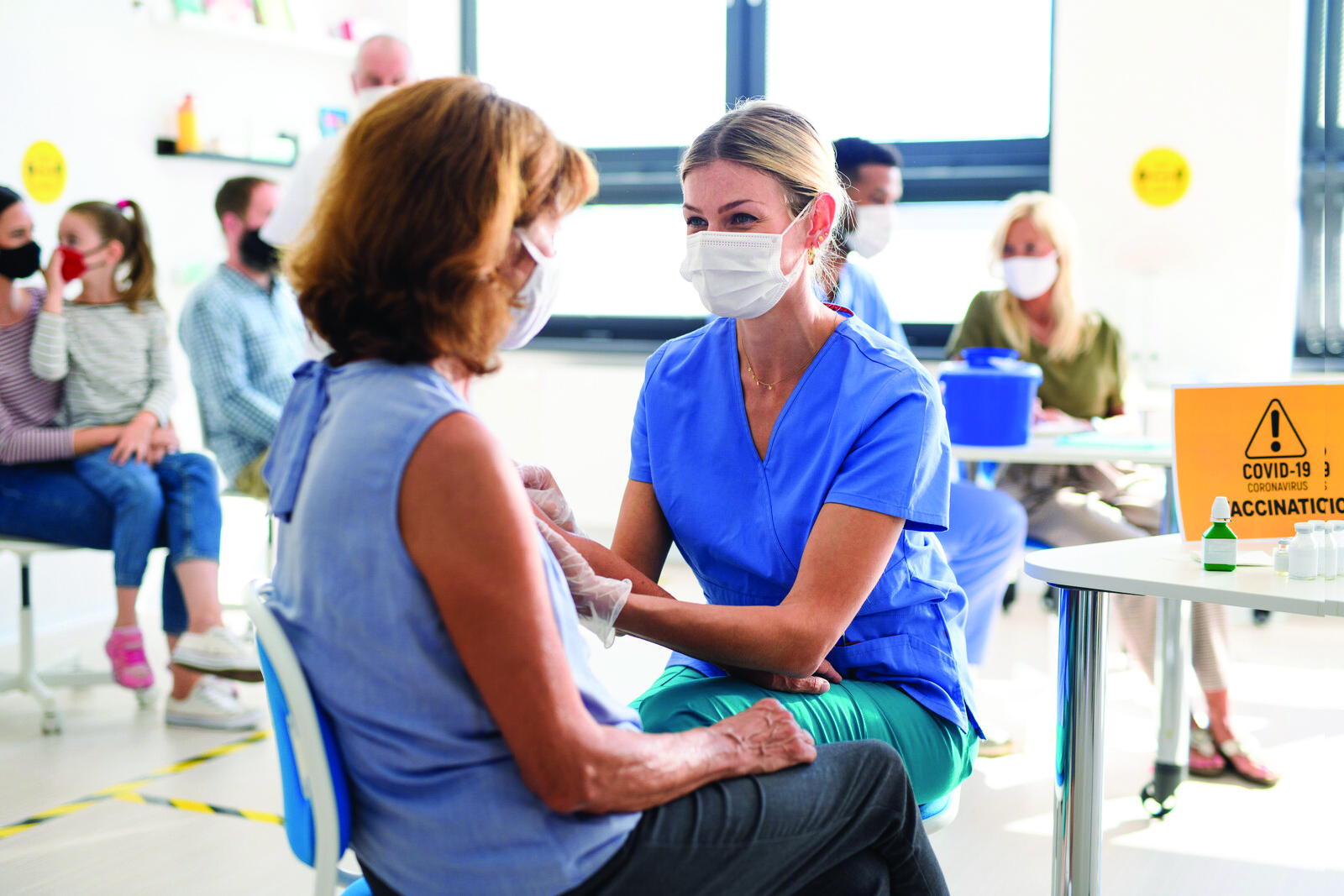
3) Making COVID-19 vaccines free reduced vaccination barriers for older Canadians
Federal, provincial, territorial, and local governments made significant efforts to provide widespread access with many jurisdictions not requiring proof of citizenship or provincial health insurance, further reducing accessibility barriers for vulnerable populations.
The opportunity: While both the influenza and pneumococcal vaccines are publicly funded in most provinces, every Canadian jurisdiction requires that older adults pay for shingles vaccines out of pocket, with the exception of Ontario who funds it for adults aged 65-70 years. Yet even in the case of influenza, only four Canadian jurisdictions make enhanced influenza vaccines available to those aged 65 years and older. The result is that many older Canadians will have to pay out-of-pocket when enhanced versions are available.
With many older adults having limited access mass vaccination clinics, several provinces and territories made additional efforts to ensure that geographic barriers were reduced. This helped enable older adults to make vaccine appointments at primary care providers and pharmacists, along with the development of vaccination strategies to better serve the homebound.
Moreover, some provinces made significant efforts to vaccinate homebound older persons using mobile clinics in self-contained vehicles.
4) Appropriate and accessible information
Some jurisdictions also made vaccine appointments more accessible by reducing communication and language barriers in English and French and booking options in dozens of languages both online and over the phone. Family members and friends could book on another’s behalf.
The opportunity: Communicating in up to 300 languages and allowing other to facilitate bookings facilitated successful vaccination uptake.
5) Integrated vaccine registries, surveillance, and monitoring of vaccination rates helped identify and target harder to reach populations
Comprehensive and integrated registration systems enabled older adults to be easily identified and booked in for their vaccination appointments in a timely manner, particularly in high-risk neighbourhoods.
The opportunity: The continuous, real-time collection of COVID-19 vaccination rates across local, provincial, and federal health authorities is a revelation compared to how influenza, pneumococcal, and shingles vaccination rates are currently captured among the general population. Today, immunization rates for influenza, pneumococcal, and shingles continue to rely primarily on surveys to predict vaccination coverage rates.
Excerpted with data from Lessons Learned: What Successful COVID-19 Immunization Efforts Taught Us About Improving Vaccine Coverage Among Older Canadians for Other Vaccine-Preventable Diseases by the National Institute On Ageing.














