Our brains have an amazing ability to grow and change. Although their most rapid development happens in early childhood and adolescence, the brain remains capable of change throughout life. This knowledge is important for healthcare professionals working in rehabilitation, mental health, chronic disease care, and community services.
Positive experiences and supportive relationships over the course of our lives helps build strong brain architecture, which in turn supports recovery, learning, and long-term health. In contrast, ongoing stress, adversity, and negative experiences can weaken brain structure and increase our individual risk of poor physical and mental health outcomes. This science reinforces the fact that health outcomes are shaped by more than injury, illness, or diagnosis alone. They are also influenced by a person’s life experiences, relationships, environment, and ability to adapt in the face of adversity. Understanding how these factors work together allows more effective, person-centred interventions that support both recovery and resilience.
The Alberta Family Wellness Initiative (AFWI)
Created by the Palix Foundation in 2007, AFWI works to address the gap between what science tells us about brain development and its impact on later life health outcomes, and how this knowledge is applied in policy and practice. While the AFWI’s first focus was on children and families, community engagement over the last two decades has shown how these core ideas are relevant across the majority of healthcare settings.
A key focus of this work has been creating shared language and understanding so that professionals from different disciplines can work together more effectively to support the individuals, families, and communities they work with. Through partnerships with the Center on the Developing Child at Harvard University, the National Scientific Council on the Developing Child, and the FrameWorks Institute, AFWI has mobilized knowledge on brain development using six simple metaphors collectively known as the Brain Story, to share this information in understandable language across settings and sectors (See image below).
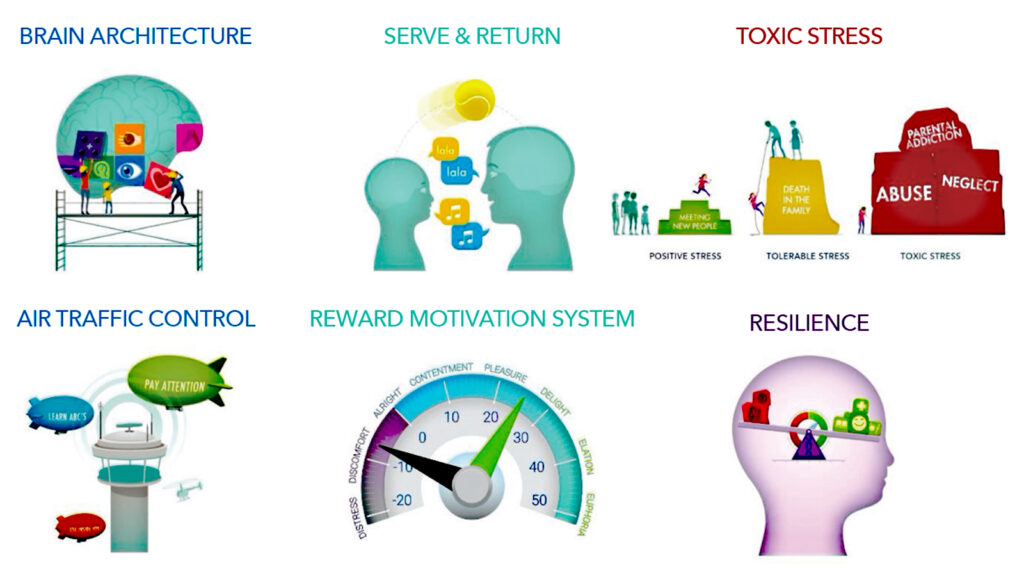
The Brain Story
The images above and below illustrate how brain development and resilience are shaped across the life course. For healthcare and rehabilitation professionals, they offer a practical way to bring brain science into assessment, care planning, and conversations with patients, families, and other providers.
— Brain Architecture. Much like a house, brains are built over time, and they require a sturdy foundation to support later development.
—The brain is built through Serve and Return interactions between a child and a caregiver. This continues into later life as interactions with other adults.
—A significant factor that undermines the brain’s foundation is Toxic Stress. These are repeated hard experiences without safe, stable relationships or environments that help a person cope. Toxic Stress makes the foundation of the house less stable and the person more vulnerable to negative outcomes.
—Air Traffic Control is a person’s ability to regulate their mental airspace by planning, organizing, paying attention, and prioritizing their activities to avoid a crash. These skills are known as executive function and self-regulation.
—The brain also has a Reward Dial, which regulates our motivation to seek out rewarding and pleasurable experiences and our responses to such experiences.
—The final metaphor brings together all the topics of the Brain Story to explain how resilience works. It is called the Resilience Scale.
The Resilience Scale
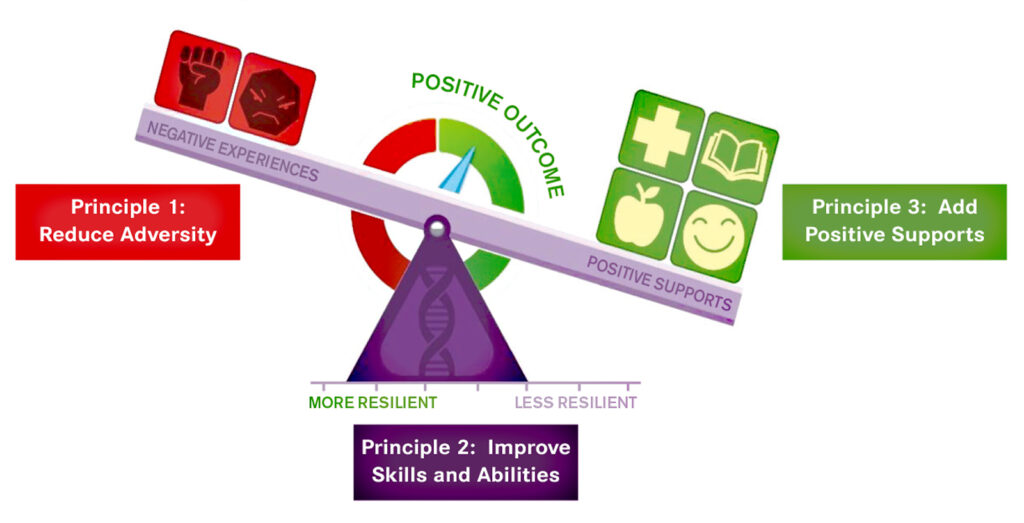
Resilience is our ability to adapt and stay healthy, even when facing tough circumstances. The Scale shows how three different factors influence our capacity for resilience: negative experiences, positive supports, and skills and abilities.
Negative experiences, sources of adversity, and ongoing toxic stress can be loaded as red boxes on the left side of the beam. If they pile up, the Scale tips towards a poor outcome marked by illness, poor recovery, and ongoing adversity.
Positive factors, which are represented by the green boxes, include safe, stable, and supportive relationships and environments. These green boxes can pile up on the right-hand side of the beam, tipping the Scale toward positive outcomes including good health and wellness.
The beam is held up by a purple fulcrum at the base which represents our skills and abilities. The purple fulcrum can move from the centre, either to the left, indicating greater capacity or to the right, indicating lower capacity for resilience. The position of the fulcrum creates more or less leverage to the boxes on each side. The starting position of our fulcrum is partly determined by our genetic disposition, but it can change over time based on our life experiences. These changes are governed by a process known as epigenetics.
Moving the purple fulcrum to the ‘more resilient’ left side is achieved through frequent opportunities to practice and use the skills and abilities of:
—Serve and return interactions
—Air traffic control
—Reward motivation
This is especially important for rehabilitation and community care, where building skills is often a key goal, alongside addressing symptoms or impairments.
Taken together, negative experiences, positive supports, skills and abilities all interact to determine whether the Resilience Scale tips toward a positive outcome or a negative outcome. It is a simple tool that helps show why people with similar health conditions or injuries can have very different outcomes. Importantly, it also shows that resilience is not fixed. It can strengthen or weaken over time depending on our experiences, supports, and skills.
Applying the Resilience Scale in Practice
Consistent, supportive relationships; access to safe, stable environments; and positive interactions within healthcare and community settings can strengthen the brain’s capacity to regulate stress, adapt to challenges, and support recovery. In rehabilitation and community care, these experiences can improve engagement, motivation, and participation in care, reinforcing the idea that how care is delivered is often as important as what care is delivered.
Programs and interventions can use the Resilience Scale to guide more targeted and coordinated care to improve outcomes for the patients they serve by encouraging care teams to think broadly about where and how to intervene for a patient using the biological underpinnings of resilience. This might include reducing sources of stress, strengthening supports, or helping individuals build skills that improve their ability to manage adversity.
The Resilience Scale can also serve as a valuable tool to help patients better understand how the factors that exist in their lives can influence their outcomes. By working with care providers to identify factors as red or green boxes, as well as the placement of the fulcrum on the Scale, patients can visualize their own capacity for resilience and how it can be strengthened by the interventions and care they are receiving.
Training opportunities
Through free in-person, virtual, or on-demand training sessions, the AFWI is working to embed this knowledge in individuals, organizations and communities. By using common language and having knowledge of brain science, healthcare professionals can improve communication, strengthen referral pathways, and better support individuals as they move between services.
Of note, the Resilience Scale Training, along with completion of a simulation activity, gives care providers the opportunity to practice using the Resilience Scale as a clinical tool. It has been approved for 2 professional learning credits by both the Royal College of Physicians and Surgeons of Canada and the Canadian Nurses Association.
Alberta Family Wellness Initiative, Palix Foundation.
To learn more, book a training session for yourself or your organization, please visit albertafamilywellness.org.
Images: iStock. Alberta Family Wellness Initiative, Palix Foundation.











