Understanding and Managing the Progression
By The Huntington Society of Canada
A rare, inherited brain disorder, Huntington disease (HD) causes the death of cells in parts of the brain (specifically the caudate, the putamen and, as the disease progresses, the cerebral cortex). There are three major areas of impact: movement, emotion and thinking. This article summarizes the various symptoms of HD, along with therapeutic options for treatment and tips for caregivers.
 Movement and speech impairment
Movement and speech impairment
Involuntary movements, defined as the diminished coordination of voluntary movements, are a common symptom of HD. People with HD may have an unsteady gait and slurred speech, which can create an appearance of intoxication. Falls are a common risk.
Options
A neurologist may advise someone with HD to have an assessment by a physiotherapist or occupational therapist, or to receive treatment to extend mobility and independence and decrease the risk of falls and injuries. A nutritionist or dietitian may also be recommended, to evaluate the affected person’s diet and suggest ways to improve nutrition and increase hydration. It is important for someone affected by involuntary movements to have easy access to high-calorie meals, drinks and supplements.
Caregiver tips
Caregivers should allow for sufficient time to support the person, providing several smaller meals if needed and creating a supportive environment by reducing disturbances and increasing comfort.
If speech impairment is a factor, a medical practitioner may suggest a speech language therapist early on.
Emotional disturbances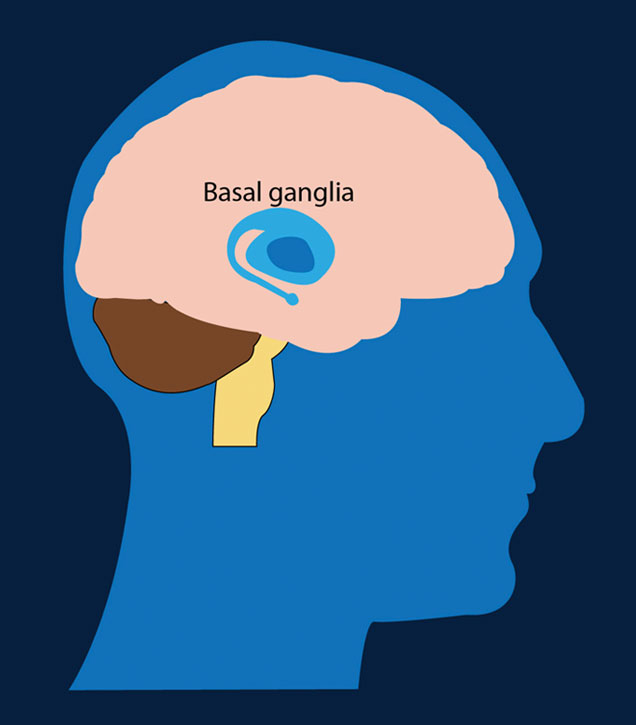
Psychiatric disorders are induced by physical changes in the brain. The affected person may suffer from depression, anxiety, suicidal ideation, psychosis, bipolar disorder, obsessive-compulsive disorder and/or sexual disorders.
Options
Caregivers will want to seek psychiatric consultation, ensure that medications are reviewed and that counseling and support are available. It is important to remember that fear and grief are common emotional reactions when diagnosed with a chronic, incurable, terminal disease. Reassurance and emotional support are key.
Caregiver tips
Sometimes those affected by psychiatric disorders exhibit repeated responses, which need to be addressed as quickly as possible to avoid an escalation to angry outbursts. Approach the individual as calmly as possible to get their attention, and use a positive response; this will help to diffuse the situation. Try to avoid confrontation or ultimatums, as these may lead to an escalation. If a person with HD is stuck on a specific idea or thought, you will not be able to reason with them or talk them out of that line of thinking. It is best to address the idea or thought, and then move on.
Not all conflicts or crises can be avoided, so set realistic goals. Be flexible and ready to try several strategies; trial and error may be necessary. Most importantly for caregivers, don’t carry the burden alone: Involve all members of the multidisciplinary care team, family members and friends.
Communications difficulties
While long-term memory remains intact in people with HD, cognitive disorder and impairment leads to difficulty with short-term memory and retrieval. The affected person may also have difficulty understanding complex information and sequencing, and have a slow response time, a short attention span and a high level of distractibility.
 Options
Options
Knowing the person with HD well will assist with communication, as sometimes the individual can only communicate through behaviour. Improving communication and comprehension can lead to a decrease in undesirable behaviour.
Caregiver tips
Communication becomes increasingly difficult as the disease progresses. In order to help manage communication throughout the disease, it is necessary for the caregiver to take responsibility for effective communication: Slow down, focus and limit distractions, keep yourself and the environment calm, and be non-judgmental. When asking questions, start with an easy question, and wait. If there is no response, that does not necessarily mean no! People with HD often take longer to provide a response. If you do not get a response, try rephrasing the question in a multiple-choice question or as a yes/no question, making sure to give adequate time for a response. If you still do not get a response, ask again later, as starting the process from the beginning at another time may make a difference.
Routines can also help to manage the disease and the expectations of both the individual affected by HD and the caregiver. Introduce daily, almost hourly, routines that meet the individual needs of the person as early as possible. Routine can lessen short-term memory deficits, distractibility, difficulty initiating or sequencing tasks, impulsivity, aggression, obsessive or intrusive thoughts, anxiety and apathy. Routines provide a sense of control and safety. Consistency comes from doing the same thing, in the same order, at the same time, in the same way, every day.
Responsive behaviour occurs when a person reacts in unusual ways to a situation that does not warrant the response (such as yelling or hitting). This is the person’s way of communicating. For example, an individual with HD may want a coffee; when the coffee doesn’t appear, he or she may exhibit responsive behaviour by yelling or hitting. Remember, people with HD do not self-regulate well. Possible causes of this type of behaviour may include inability to communicate; unawareness of limitations and/or needs of others; boredom or feeling overwhelmed by overtaxing tasks; a change in routine; noise; and feelings of frustration, fear and grief. People with HD also have an inability to self-regulate when experiencing physical discomfort such as pain, hunger, thirst, tiredness, or feeling too hot or cold.
Try to determine the root of the issue and what the person is trying to communicate. Here are some tips to help you observe, gather and share information:
1. When does the challenging behaviour not occur?
2. Where does the client have a good time, and with whom?
3. What conditions offer opportunities that seem to determine a “good time”?
4. When and where does the challenging behaviour occur? What precedes it and who is involved?
5. What emotion was expressed?
6. What seemed to trigger the challenging behaviour? The more you can observe, gather and share information, the more support you can provide.
7. What intervention supported the person in calming down?
8. What action was counterproductive? Identifying both the positive exceptions and the triggers for challenging behaviours will allow you to adapt environments, time frames, schedules, approaches and goals in ways that provide the most supportive conditions so future crisis can be avoided.
In summary, the caregiver is the foundational support for the person affected by HD. Whether you are an informal caregiver or a health professional, we encourage you to work in close cooperation with other caregivers, medical personnel and staff involved in the care of the individual with HD.
By communicating effectively with all involved, you have the opportunity of providing a high quality of life for as long as possible. We suggest using journals to share observations. Spend as much time as possible with the individual during a good period. Always remember that the person living with HD does not have any control over physical, emotional and cognitive changes. Accept that unintentional, “non-compliant” behaviour is part of HD. Take on the challenge of responsive behaviour; the person with HD cannot simply try harder, but we can understand the progression of the disease and manage accordingly.
The Huntington Society of Canada provides information to help caregivers and health professionals cope with the complexities of the disease while caring for someone who is affected by one or more of these areas of impact. For more information, please visit www.huntingtonsociety.ca.