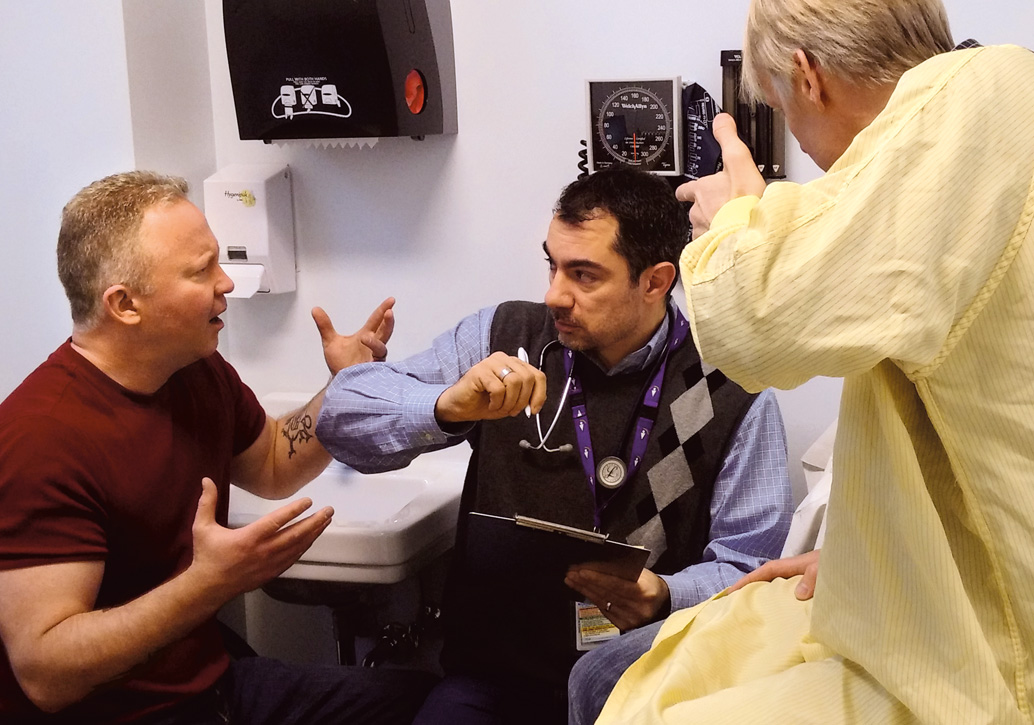
Then and Now: Violence Prevention Exercises
By Gail Allison, Conor MacPhee and Heather Noullett
Violence is a pervasive problem in health care settings, affecting both frontline workers and employers. The BC Provincial Violence Prevention Steering Committee defines workplace violence as “incidents where people are abused, threatened or assaulted in circumstances related to their work, involving a direct or indirect challenge to their safety, well-being or health.”
In BC, health care workers account for 11 per cent of the workforce and 57 per cent of all violence-related time-loss claims. Prevention and management of violence require a genuine commitment at the organizational level and cooperation to assess needs and implement change; staff education and training is one of the most important components. In 2015, the Violence Prevention Specialist (VPS) team at Vancouver Coastal Health developed a scenario-based simulation training program called Violence Prevention Exercises (VPE) to enhance the existing Provincial Violence Prevention Curriculum (PVPC), which consists of online modules and classroom instruction.
The goal of the training was to reinforce the concepts and principles introduced in the classroom, and to increase the confidence of staff in dealing with real conflict situations. The use of simulation provides a practical application and gives staff the opportunity to “train their brains” and practice recognizing and adapting to changes in themselves, their environment and their patients.
What is being done?
We have introduced the VPE program to more than 40 sites across Vancouver Coastal Health, including the GF Strong Rehabilitation Centre and several community-based programs covering public health, mental health and substance use, and home care. VPEs are delivered to small multidisciplinary groups of staff in 30-minute sessions, and include an introduction, the development of a scenario, a simulation, a debriefing and wellness check. Rehabilitation staff frequently suggest scenarios that are centred on aggression arising from their patients’ complex circumstances, including pain, slow progress, limited mobility, drug and alcohol use, and loss of independence. Site-specific applicability is a crucial element of the VPEs, so participants are prompted to craft a scenario at the beginning of each session. As we developed the program, we discovered that one of the most significant factors in staff engagement and retention was participation—when staff crafted their own scenario for the simulation they were more engaged, as compared with when the scenario was provided by the facilitator.
After developing a scenario, staff participate in a brief simulation led by a VPS. In most simulations, the VPS plays the role of the patient to ensure fidelity. During the simulation, staff use the skills learned in the classroom portion of the PVPC, such as de-escalation strategies, personal space management, recognition of pre-incident indicators and when to call for help. The simulations are designed to conclude with a successful de-escalation or safe disengagement.
Identifying gaps
In addition to allowing the practise of violence prevention skills, VPEs also offer an opportunity to reinforce corporate policies and local procedures. This is particularly valuable for staff who work in community settings and who do not have the infrastructure that exists in acute care settings, such as duress alarms, immediate peer support and security. Furthermore, the VPS can identify gaps in staff awareness of safety procedures, such as reviewing the community risk screen, knowing how to call for help and understanding how to check in when working alone. When knowledge deficits become apparent, the VPS can support staff learning by reviewing the site procedures.
As we rolled out the program, it became evident that the need to attend to emotional wellness related to violence was more significant than we had initially anticipated. During many VPEs, staff disclosed incidents of violence that continued to affect their psychological well-being. In many cases staff expressed feeling unsupported, which resulted in loss of trust within the team, and feelings of fear and inadequacy. In response, we engaged a clinical counsellor to support the exercises in one of our high-risk units. The counsellor attended and co-facilitated with the VPS, with a focus on managing the psychological effects of workplace violence and making use of organizational resources such as peer support, counselling and critical incident stress management. Furthermore, the VPEs allowed us to remind staff about the requirement for and importance of reporting incidents of violence through the organization’s reporting structure.
Preventing skill decay
We piloted the program in six sites in spring 2015. Feedback from staff, managers and physicians was very positive, and interest was quickly generated among other sites via word of mouth. VPEs became a core part of our work and we prioritized implementing them in additional units over the following months. In early 2017, a BC provincial working group was established with representatives from health employers and unions. The group’s mandate was to develop a sustainability model for the classroom education to prevent skill decay using simulation-based learning. Given the evidence in support of simulation-based learning and the success of the VPEs, the working group adapted our model as a mandatory component of the PVPC. The group developed instructional materials, including a list of nine debriefing questions that were designed to lead a group through a debriefing after a simulation and to reinforce all of the competencies first introduced in the classroom. As of January 2018, the VPEs (now known as PVPC refresher training) have been implemented in all health authorities in BC.
A culture of safety
The process of developing and implementing the VPEs and then formalizing the refresher training has been very rewarding for our team. Both the VPS team and the staff we serve have experienced the benefits of increased face-to-face interaction, which allows for enhanced learning opportunities and stronger relationships. Delivering this education at the worksite gives us an opportunity to regularly engage with frontline workers, clinicians, physicians and leaders to support them in embedding a culture of safety.
Gail Allison, RN, BHScN, MA, CRRN, is Director of Safety & Prevention, Workplace Health, Vancouver Coastal Health.
Conor MacPhee, MA, and Heather Noullett, BA, are VPSs at Vancouver Coastal Health.